In February 2020 I published a blog posting – Emerging Pathogens, Communications – that encapsulated my observations and learnings from my years work in the early years of the HIV/AIDS pandemic in the early 1980s. As we sit, possibly, on the cusp of another large scale medical challenge with monkeypox, it seemed like a good idea to revisit the topic. When there is a new and scary thing we are facing, medically speaking, there are some truisms regarding the communications environment that can inform strategic thinking about how we talk about it.
- Facts are low, speculation is high – And nature hates a vacuum and there will be many who are willing to fill the void with misinformation. People want facts, and the fact is, facts are in short supply.
- Numbers don’t mean a lot – First of all, they change quickly – and are changing very quickly with monkeypox. In addition, there is often a lack of accurate reporting for many reasons.
- Points of reference will change – What we know, and what we don’t know, will change over time as we get more experience and gain wider understanding. That might seem like a good thing, but in fact, changing stories undermine credibility.
- Fraud potential is high – There are people who will take advantage of the situation and exploit it for political and/or financial gain. That, too, impacts credibility and can confuse people.
- Policy is likely to be ham-handed – Policies may be developed quickly and without adequate information and be based on emotion and bias more than facts. This is another factor that strains credibility.
Monkeypox is not COVID, and COVID was not AIDS. They each present distinct challenges and evoke particular fears and concerns. There are big differences between the three. But they are all viruses. And when it comes to communications challenges there are many commonalities.
First and foremost, in the absence of facts, fear can drive actions. And when a pathogen is newly emerging, facts are greatly outnumbered by questions. The degree to which companies, educators, businesses and service providers may want to prepare to deal with those challenges may depend on where they are, who their stakeholders are, and how big or small they are. At this stage though, better to consider the challenges that may lay before you know, before they present themselves.
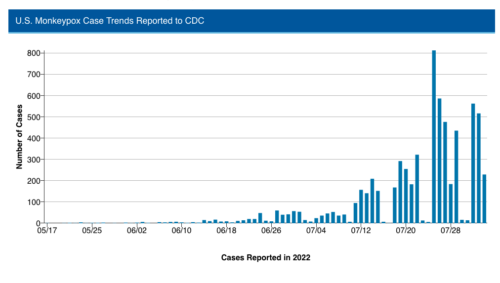
Analysis
It may be that monkeypox is contained early if we are lucky. There are reported signs that transmission may be slowing in the U.K. and the trend in the graph above appears to show some deceleration. That said, the numbers have increased quickly on an extremely steep curve. That means there is an increasing amount of virus out there. The virus has mainly spread among men who have sex with men and transmission is being attributed to skin contact. But the higher the numbers go the greater potential there is for more lateral spread. A presumptive pediatric case was reported last week in California. It is also a virus that can move between people and animals.
Containment depends on systems that are able to screen, test, treat, and prevent (both by means of avoiding circumstances that can enhance transmission and by vaccination). To that end, many things are not in our favor. An extremely splintered approach at federal, state and local levels impacts the coordination of a public health response. We have COVID fatigue in the extreme. And in terms of tools, we do not have a means for screening, meaning we do not know who is infected before they exhibit symptoms which may take several days; the testing situation is complicated because there is no quick, at-home testing like there is for COVID and may be best applied when there are lesions. But people may have other symptoms such as headache, chills, muscle aches, swollen lymph nodes and exhaustion. The only FDA-approved drug to treat is approved for smallpox, but no Monkeypox and has been difficult to access. In terms of prevention, while a vaccine has been developed, supply is very short and it, too, has been hard to get.
Additional challenges include the fact that the course of illness runs two to four weeks. If a person must self-isolate for that length of time it is not only difficult, but there may be collateral consequences. With men who have sex with men comprising the overwhelming majority of cases, a diagnosis is the equivalent of coming out. For many gay men that is not a problem. For many others, who may have wives and children, it can be a very large one, facing a situation that may have both personal and professional peril.
At the present time, there are some states which are reporting higher numbers than others. If the numbers do continue to climb, then a larger number of geographies will be impacted and most likely a wider circle of people, raising the chances that large employers, those in specific sectors, may face communications challenges sooner rather than later such as:
- Travel and hospitality
- Schools and universities
- Hospitals
- Institutional settings such as daycare centers, rehab and nursing homes (a case of a daycare workers was reported in Illinois last week)
What to Do
Every business, service or place of public accommodation is different. There is no one-size-fits-all approach to preparation. One must consider the size of the enterprise, the stakeholders and the level of physical contact and interaction with surfaces. That said, there are echos from both AIDS and COVID that shed light into how people may react to the emergence of another communicable condition. A few things to consider:
- Review policies and assess what may need to be changed or amended; this is not just COVID return-to-work policies, but discrimination policies as well. Re-think many of the things you have had to communicate about a virus transmitted by air, and re-fashion to think about surfaces. Monkeypox will present distinct challenges.
- Consider the questions and issues you may face. Can we catch monkeypox using the toilet? Trying on clothes? Do I have to sit next to the gay man? My co-worker says it is eczema, I’m afraid it is Monkeypox. Depending on your business, your clientele, there are different sets of questions that may arise for different settings. Think about what they might be and to what degree you are the one to have to provide the answers.
- Assess the triggers for potential fear and conflict between employees, customers and users of any service.
- Communicating in an environment where what we know changes, and what was certain yesterday may be uncertain tomorrow is always a strain on credibility. Therefore consider integrating reminders to that effect in your messaging. What we know now is….
- Gather reliable resources – the obvious ones such as CDC, FDA, and Departments of Health at the state and local levels, but also consider credible grassroots organizations, particularly ones that may resonate with stakeholders, particularly those dealing with gay-related health issues and key medical societies such as the American Society for Microbiology and others.
Many people think that preparation during such a nascent phase of the outbreak is over-reacting. I hope they are right. But having lived through AIDS and COVID, and seen early numbers quickly spell a different story over a very short period of time, one may be well-served to think it through now.

